Clean Room techology
Opremanjem novog laboratorija pomno je odabran svaki detalj kako bi se povećale šanse za trudnoću. Laboratorij je smješten u sredini novog prostora, izoliran od svih ostalih prostorija zračnom bravom, zidovi su izrađeni od antibakterijskih ploča koje se koriste u tehnologiji čistih soba, a boje i ljepila koja se koriste u gradnji odabrana su tako da sadrže minimalne količine otrovnih tvari.
Prednosti tehnologije čiste sobe u odnosu na konvencionalne IVF laboratorije
- prostori laboratorija se zagrijavaju i zrak u njima se kontinuirano filtrira 8 tjedana (tzv. burn out) uklanjajući sve moguće tragove otrovnih spojeva
- Tri serije vanjskih filtera i jedan unutarnji filter čiste zrak od prašine, smoga, spora, bakterija, virusa i organskih tvari
- Pročišćeni zrak pod tlakom od 20 Ps uvodi se u laboratorij sa 20-30 izmjena zraka na sat
- Prostorije uz laboratorij imaju niži tlak pročišćenog zraka tako da zrak uvijek izlazi iz laboratorija
Svim ovim modernim tehnikama pružamo najbolje moguće okruženje za uspjeh embrija.
MACS – magnetsko sortiranje stanica s aneksinom V konjugiranim mikrozrncima
Priprema sjemena pomoću magnetskog sortiranja stanica s ranim znakovima oštećenja
Fragmentacija DNK jedan je od nevidljivih znakova propadanja sperme. Takve sperme ne možemo razlikovati od drugih dok se ne obojaju na određeni način što nam pomaže da dijagnosticiramo njihov povećani udio, ali nakon toga ne možemo koristiti preostale zdrave stanice u terapiji npr. inseminacijom ili u postupku IVF-a.
Prednosti MACS-a:
- Oštećeni spermij može se vrlo rano prepoznati i izolirati
- Ova metoda povećava uspješnost oplodnje i kvalitetu embrija u vantjelesnoj oplodnji
HBA test i PICSI metoda
Ovim se testom utvrđuje zrelost sperme u izvornom uzorku sjemena (prije bilo kakvog tretmana koji odvaja spermu s najboljim karakteristikama). Test se temelji na sposobnosti zrelih spermija da se vežu na hijaluronan, spoj koji se nalazi u visokim koncentracijama u folikularnoj tekućini u kojoj se jajašce razvija i cumulus oophorus, skupini stanica i međustaničnoj tvari koja okružuje jaje.
Spermije koje se vežu za hijaluronane:
- Utvrđeno je da takvi spermiji imaju bolju morfologiju i 4-6 puta manje kromosomskih aneuploidija
- Veće šanse za uspješnu oplodnju
- Kombinacija dviju metoda (MAC i PICSI) daje izvrsne rezultate.
Vitrifikacija
Metoda pohranjivanja jajnih stanica i embrija u kojoj se uzorak uranja izravno u tekući dušik na -196°C, što dovodi do “glazure” tekućeg dijela stanica, tzv. vitrifikacije.
Najvažnija prednost ove metode:
- Kristali leda ne nastaju kao kod sporog smrzavanja, u kojem se voda pretvara u kristale koji mogu mehanički oštetiti smrznuti materijal
- Uvođenjem ove metode krioprezervacije, preživljavanje jajnih stanica poraslo je na 90-100%.
Halosperm – test fragmentacije DNK
Fragmentacija DNK spermija prirodna je i normalna pojava koja se javlja kao posljedica programirane smrti spermija (apoptoze) i ako se primijeti u približno 30% spermija nema značajan utjecaj na plodnost muškaraca.
Fragmentacija DNK spermija jedan je od prvih znakova propadanja spermija i ne može se povezati s uobičajenim parametrima analize sjemena kao što su broj, koncentracija i pokretljivost spermija.
Ovaj test je izuzetno koristan i pomaže u davanju odgovora na sljedeća pitanja:
- koji su parovi prikladni za AIH (Inseminaciju)
- treba li se na IVF primijeniti modificirani pristup (ICSI, PICSI, IMSI).
- je li operacija varikokele bila učinkovita
- kolika je šteta prouzročena infekcijom klamidijom i mikoplazmom
- zbog čega se neuspjeh MPO postupaka ponavlja kod nekih parova
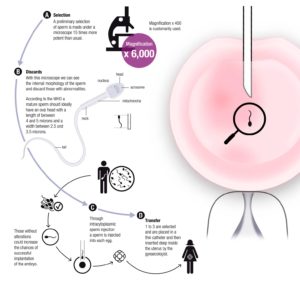
IMSI postupak
Od samog početka liječenja muške neplodnosti mikromanipulacijskim metodama, jedan od glavnih problema je izbor sperme.
Kako bi se spriječila selekcija potencijalno neprikladnih spermija za oplodnju i pravilan embrionalni razvoj, potrebno je primijeniti metodu MSOME (motile sperm organelle morphology ispitivanje), pri čemu se spermij uočava u porastu od 6.000 do 13.000 puta.
Kako se radi o neobojenom preparatu, te živim i pokretnim spermijima, primjena ove metode u klinici dovela je do razvoja modificirane varijante ICSI pod nazivom IMSI (intracitoplazmatska morfološki odabrana injekcija spermija) kojom odabiremo morfološki najbolje spermije.
Kombinacija PICSI i IMSI metoda daje najbolje rezultate u slučajevima bračne neplodnosti uzrokovane muškim faktorom.